(1).gif)
(1).gif)

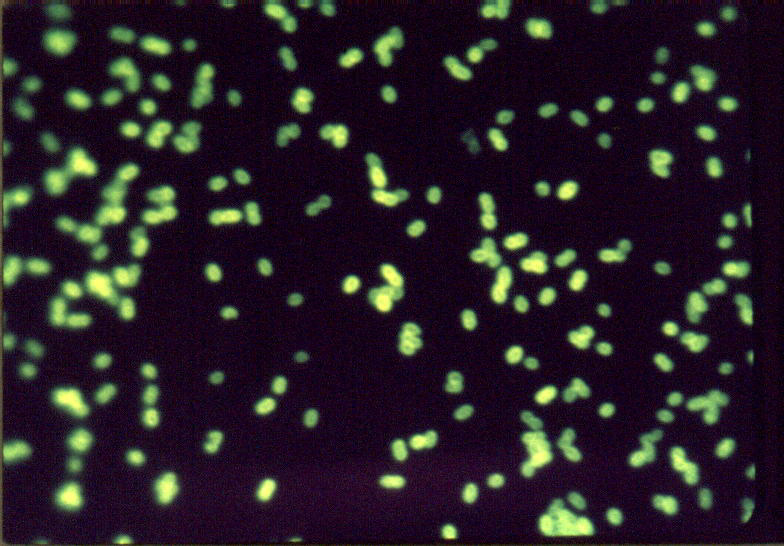
Enterococcus spp.viewed by direct fluorescent antibody (FA) reaction
![]() Enterococcus
faecalis and Enterococcus faecium: Most common, clinically relevant
intestinal species
Enterococcus
faecalis and Enterococcus faecium: Most common, clinically relevant
intestinal species
![]() Previously
(1984) classified as Group D streptococci: Possess
a Group D specific cell wall carbohydrate (glycerol teichoic acid linked to
cytoplasmic membrane)
Previously
(1984) classified as Group D streptococci: Possess
a Group D specific cell wall carbohydrate (glycerol teichoic acid linked to
cytoplasmic membrane)
![]() Nonmotile
Gram-positive cocci in pairs or short chains (see WebLinked
image): Difficult to distinguish from S. pneumoniae
Nonmotile
Gram-positive cocci in pairs or short chains (see WebLinked
image): Difficult to distinguish from S. pneumoniae
![]() Catalase
negative
Catalase
negative
![]() Most
are facultative anaerobes
Most
are facultative anaerobes
![]() Complex
nutritional requirements (fastidious)
(blood or serum required)
Complex
nutritional requirements (fastidious)
(blood or serum required)
![]() Fermentative
metabolism (carbohydrates to lactic acid)
Fermentative
metabolism (carbohydrates to lactic acid)
![]() Halotolerant
and bile resistant (adapted to niche
in intestinal environment)
Halotolerant
and bile resistant (adapted to niche
in intestinal environment)
![]() Lancefield
group D specific teichoic acid antigen
Lancefield
group D specific teichoic acid antigen
![]() Important
life-threatening nosocomial infections:
Vancomycin Resistant Enterococci (VRE) are one of most important nosocomial
pathogens of the 1990s
Important
life-threatening nosocomial infections:
Vancomycin Resistant Enterococci (VRE) are one of most important nosocomial
pathogens of the 1990s
![]() Urinary
tract infections
Urinary
tract infections
![]() Wound
infections and intrabdominal abscesses are generally polymicrobial
Wound
infections and intrabdominal abscesses are generally polymicrobial
![]() Foodborne
disease
Foodborne
disease
![]() Meningitis
Meningitis
![]() Inhabit
the intestines of humans and animals
Inhabit
the intestines of humans and animals
![]() Typically
commensals: Capable of
surviving in high concentrations of bile and sodium chloride
Typically
commensals: Capable of
surviving in high concentrations of bile and sodium chloride
![]() E.
faecalis colonize the large intestine (~107 organisms
per gram of feces) and urinary tract
E.
faecalis colonize the large intestine (~107 organisms
per gram of feces) and urinary tract
![]() E.
faecium colonize similar sites in lesser numbers
E.
faecium colonize similar sites in lesser numbers
![]() Most
infections originate from an intestinal site: Transmission also seen person-to-person
and through consumption of contaminated food
Most
infections originate from an intestinal site: Transmission also seen person-to-person
and through consumption of contaminated food
![]() Risk
factors for enterococcal infections:
Risk
factors for enterococcal infections:
Urinary or intravascular catheterization
Long-term hospitalization with broad-spectrum antibiotics
![]() Broad
range multidrug antibiotic resistance: Mediated by R-plasmids that
are "promiscuously" passaged between bacteria
Broad
range multidrug antibiotic resistance: Mediated by R-plasmids that
are "promiscuously" passaged between bacteria
![]() No
single potent virulence factor: Colonization and secreted factors
No
single potent virulence factor: Colonization and secreted factors
Fibrinolytic
Protein and carbohydrate factors: Regulate adherence
Bacteriocins: Inhibit competitive bacteria
![]() Large
white colonies
Large
white colonies
![]() Typically
nonhemolytic, but may be alpha- or beta-hemolytic
Typically
nonhemolytic, but may be alpha- or beta-hemolytic
![]() Resemble
S. pneumoniae in Gram stains
Resemble
S. pneumoniae in Gram stains
![]() Resist
heat (60o C for 30 minutes)
Resist
heat (60o C for 30 minutes)
![]() Most
capable of growing:
Most
capable of growing:
from 10o to 45oC range; optimal growth at 35oC on nonselective agar (blood or chocolate agar)
in 0.1% methylene blue milk
in 40% bile salts (bile tolerant); colonies do not dissolve when exposed to bile (differentiates from S. pneumoniae)
in 6.5% NaCl concentration (halotolerant)
![]() Readily
distinguished from other a-hemolytic
or g-hemolytic (nonhemolytic) Streptococcus spp. by:
Readily
distinguished from other a-hemolytic
or g-hemolytic (nonhemolytic) Streptococcus spp. by:
growth on Bile Esculin Agar (BEA) slants with blackening of the medium due to hydrolysis of esculin to esculetin
production of acid from several sugars, including glucose, maltose and lactose
growth in SF broth (Streptococcus [Enterococcus] faecalis broth) with production of acid
resistance to optochin (differentiates from S. pneumoniae)
Hydrolysis of pyrrolidonyl-beta-naphthylamide (PYR) (differentiates from S. pneumoniae)
![]() Antibiotic
resistance makes treatment difficult
Antibiotic
resistance makes treatment difficult
![]() Synergistic
combination: Aminoglycoside and cell wall-active antibiotic (e.g., ampicillin,
vancomycin)
Synergistic
combination: Aminoglycoside and cell wall-active antibiotic (e.g., ampicillin,
vancomycin)
(1).gif) Go to Pathogen List
Go to Pathogen List| Lecture Syllabus | General Course Information | Grade Determination |
| Laboratory Syllabus | Interesting WebSite Links | Lab Safety |