
(1).gif)
(1).gif)

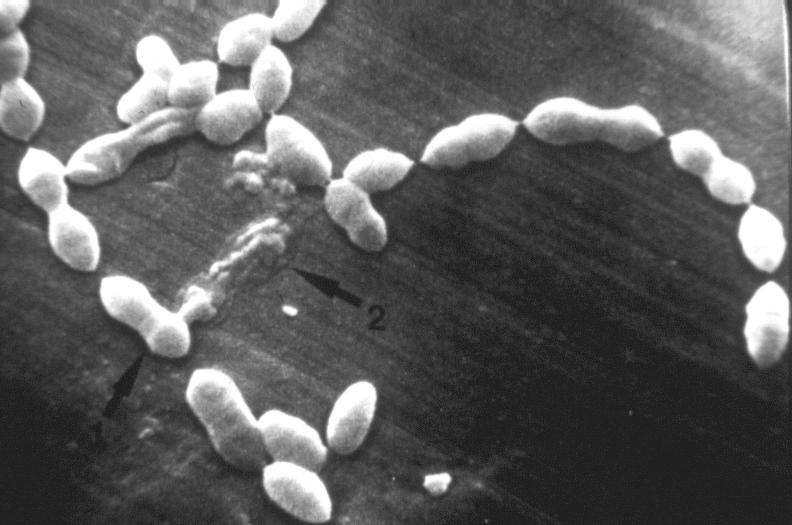
Click Here to View More Images of Streptococci
![]() General
Characteristics:
General
Characteristics:
Gram-Positive, Nonmotile Cocci (0.5-1.2um) often Arranged in Pairs or Chains (see WebLinked image; see WebLinked image)
Exist as Commensals and Parasites for Man, Animals or Saprophytes
Most are facultative anaerobes
Complex nutritional requirements (fastidious): Require blood- or serum-enriched media; Inability to synthesize many basic building blocks
Fermentative metabolism: Carbohydrates are fermented without the production of gas; Major endproducts are lactic acid, ethanol, acetate
Catalase negative: Useful to distinguish streptococci from staphylococci
Oxidase negative
Rigid cell wall with typical Gram-positive peptidoglycan layer, inner plasma membrane, mesosomal vesicles, nucleoid; Divide by crosswall septation
Some strains have hyaluronic acid capsule; Produce hyaluronidase later in growth cycle
![]() Cellular
Structure of Group A Streptococci: S. pyogenes
Cellular
Structure of Group A Streptococci: S. pyogenes
Cell wall contains group- and type-specific antigens
Group-specific carbohydrate (C-polysaccharide):
- ~10% dry weight of the cell
- Branched polymer of L-rhamnose and N- acetyl-D-glucosamine (2:1 ratio); latter is antigenic component; linked by phosphate-containing bridges to peptidoglycan which is composed of N-acetyl-D-glucosamine, N- acetyl-D-muramic acid, D-glutamic acid, L- lysine, and D- and L-alanine
Type-specific proteins: Two major classes, M and T antigens; Minor classes include: F, R and M-like or M-associated proteins (MAP) antigens
- M Protein: Fimbriae-like, "hairy" extensions associated with virulent strains
- Resistant to heat and acid; Trypsin sensitive
- Carboxy (-COOH) terminal end of molecule is anchored in cell wall and sequence is highly conserved among all M serotypes
- More than 80 M serotypes are due to antigenic diversity of the M protein's amino (-NH2) terminus which is surface-exposed
- T protein: Useful epidemiological marker; Not identified as virulence factor
- Trypsin resistant; Resistant to heat and acid
- M-like proteins: Structurally similar to M protein
- F protein: Binds fibronectin
- Lipoteichoic acid is also antigenic
Capsular polysaccharide: composed of hyaluronic acid (also found in host connective tissue)
![]() Based
on biochemical (Physiological) properties
Based
on biochemical (Physiological) properties
![]() Based
on clinical presentation:
Based
on clinical presentation:
Pyogenic (suppurative)
Oral
Enteric
![]() Based
on hemolytic patterns:
Based
on hemolytic patterns:
Beta-hemolytic: beta-hemolysis often enhanced under anaerobic conditions
Alpha-hemolytic
Gamma-hemolytic
![]() Based
on serology: Lancefield serogrouping
of beta-hemolytic streptococci; Lancefield group-specific antigens
Based
on serology: Lancefield serogrouping
of beta-hemolytic streptococci; Lancefield group-specific antigens
Lancefield (1933) developed useful serotyping system for classification of beta-hemolytic streptococci based on the group-specific antigenic composition of cell wall carbohydrates (Note: viridans streptococci and Streptococcus pneumoniae have no group-specific antigen)
Serogroups A through H and K through V
Major pathogens
- Group A Streptococci: Streptococcus pyogenes
- Group B Streptococci: S. agalactiae (Note: May also be alpha-hemolytic or nonhemolytic)
- Enterococcus faecalis and E. faecium were previously classified as Group D streptococci
Common pathogens
- Group C Streptococci: S. equismilis (pharyngitis); S. anginosus (abscess formation)
- Group F Streptococci: S. anginosus (abscess formation)
- Group G Streptococci: S. anginosus (abscess formation)
Uncommon pathogens
- Group D Streptococci: S. bovis, S. durans, S. avium (foodborne disease)
- Groups E, H, and K through
Streptococci lacking group-specific antigens
Viridans streptococci: Gamma or alpha-hemolysis
- Streptococcus mutans group
- S. sanguis group
- S. salivarius group
- S. mitis group
- S. anginosus-milleri group
- Streptococcus spp.
Streptococcus pneumoniae
![]() Group
A Streptococcus (S. pyogenes): One of the most important human
pathogens; Commonly associated with a diverse group of human diseases, including
both suppurative (pus-forming)
and nonsuppurative diseases
Group
A Streptococcus (S. pyogenes): One of the most important human
pathogens; Commonly associated with a diverse group of human diseases, including
both suppurative (pus-forming)
and nonsuppurative diseases
Suppurative streptococcal diseases (Acute streptococcal infection)
Pharyngitis (& tonsilitis): "strep throat" --- Suffix "-itis" refers to inflammation of (in this case, inflammation of the pharynx or tonsils)
Scarlet fever: complication of streptococcal pharyngitis when infecting strain is lysogenized ; Frequently develop scarletina rash on upper chest spreading to extremities
Cutaneous & soft tissue infections:
- Pyoderma (Impetigo: contagious pyoderma with superficial yellow weeping lesions)
- Erysipelas: Acute superficial cellulitis of skin with lymphatic involvement; face and lower extremities, skin and subcutaneous tissues
- Cellulitis: Involvement of deeper subcutaneous tissues; Deeper invasion with systemic symptoms
- Necrotizing fasciitis (a.k.a., "flesh-eating bacteria"): Infection deep in subcutaneous tissues that spreads along fascial planes, destroying muscle and fat; Initially cellulitis followed by bullae (fluid filled blisters; bulla is singular), gangrene, systemic toxicity, multiorgan failure and mortality in more than 50% of patients
- Streptococcal toxic shock syndrome: Multisystem toxicity following soft tissue infection progressing to shock and organ failure (not to be confused with Staphylococcal Toxic Shock Syndrome where hyperabsorbent tampons have been identified as an important risk factor); Systemic infection following soft tissue infection
Other suppurative diseases: Puerperal sepsis (associated with childbirth); Lymphangitis (inflammation of lymphatic vessel(s)); Pneumonia
Bacteremia: bacteria in the blood with mortality approaching 40%; Septicemia (sepsis): systemic disease associated with persistent presence of bacterial cells, bacterial toxins or other bacterial products in the blood
Acute nonsuppurative (non-pus-forming) sequelae (complications) of Group A streptococcal disease: Post-infection sequelae
Acute rheumatic fever (ARF): Inflammation of heart, joints, blood vessels, subcutaneous tissues
- Nonsuppurative inflammatory reaction characterized by arthritis, carditis, chorea (disorder of nervous system with involuntary spastic movements), erythema marginatum (skin redness with defined margin), or subcutaneous nodules
- Morbidity and mortality linked to subsequent valvular heart disease
- Poorly understood pathogenesis with several proposed theories including cross-reactivity of heart tissues and streptococcal antigens, exotoxins, or direct invasion
Rheumatic heart disease: Chronic, progressive heart valve damage
Acute glomerulonephritis: Acute inflammation of renal (kidney) glomeruli
- Signs include dark, smoky urine with RBC's, RBC casts, white blood cells, depressed serum complement, decreased glomerular filtration rate
- Granular accumulations of immunoglobulin due to deposition of immune complexes within the kidney
![]() Group
B Streptococcus (S. agalactiae)
Group
B Streptococcus (S. agalactiae)
Neonatal disease (Early onset and late-onset): Infection can occur in utero, at birth, or during first few months of life
Neonatal sepsis (septicemia)
Meningitis: Inflammation of the meninges
Pneumonia
Obstetric complications:
Urinary tract infections (UTIs)
Peurperal (postpartum) sepsis
Amnionitis: Inflammation of amnion (membrane enveloping fetus)
Endometritis: Inflammation of the endometrium (inner mucous membrane of the uterus)
Wound infections
Infections in non-pregnant adults: Primarily skin and soft tissue involvement
Genitourinary tract infections (urosepsis)
Wound infections
Pneumonia
Bacteremia
![]() Other
Beta-Hemolytic Streptococci:
Other
Beta-Hemolytic Streptococci:
Most commonly Group C (S. equisimilis, S. anginosus), Group F (also S. anginosus), and Group G (also S. anginosus)
Pharyngitis
Abscess formation
Bacteremia
Group D: Foodborne disease similar to staphylococcal intoxication
![]() Non-Beta-Hemolytic
Streptococci: Viridans Streptococci (heterogeneous collection of alpha-
and non-hemolytic)
Non-Beta-Hemolytic
Streptococci: Viridans Streptococci (heterogeneous collection of alpha-
and non-hemolytic)
Dental caries (cavities): S. mutans adhere to enamel via production of insoluble dextran from glucose; Allows other organisms to adhere (plaque formation) with acid production causing tooth decay; Lactobacillus spp. cause caries of dentin secondary to enamel caries caused by mutans streptococci (see also Actinomyces)
Subacute bacterial endocarditis: S.mutans, S. sanguis adhere to previously damaged heart valves via production of insoluble dextran from glucose
Abscess formation (suppurative intraabdominal infections)
![]() General
Overview:
General
Overview:
Streptococci have a predilection for the upper respiratory tract or skin; Strains that colonize the skin are usually different "antigenic types" from those that colonize the throat
Group A streptococci commonly colonize the oropharynx of healthy children and young adults or the skin
Colonization is transient due to development of M protein-specific immune response
Rapidly killed after phagocytic ingestion, but cell walls that are not digested may lead to chronic inflammatory lesions
Elevated incidence of carriage
Non-beta-hemolytic streptococci are competitive; Produce bacteriocins which are inhibitory to Group A strains
![]() Acute
Streptococcal Infection: Disease from recently acquired strain
Acute
Streptococcal Infection: Disease from recently acquired strain
Pharyngitis (peak ages 5-15 years) and scarlet fever (complication of streptococcal pharyngitis):
Transmitted person-to-person by droplets from respiratory secretions; Crowding increases risk (e.g., classrooms, day care facilities)
Acute rheumatic fever and glomerulonephritis sequelae to pharyngitis
Scarlet fever results from infection with a strain that is lysogenized with a temperate bacteriophage that genetically encodes for pyrogenic exotoxin (formerly known as erythrotoxin or erythrogenic toxins)
Cutaneous & soft tissue infections:
Transmitted through breaks in skin after direct contact with infected person, fomite, or arthropod vector
T-antigen typing useful where non-M typeable
Only glomerulonephritis sequelae
Streptococcal toxic shock syndrome: caused by different M serotypes than those causing pharyngitis; pyrogenic exotoxins, particularly exotoxin A, are produced
Neonatal and puerperal disease:
Transient colonization of vagina observed in both pregnant and nonpregnant females, most commonly by limited number of serotypes
Colonize lower gastrointestinal (GI) tract and genitourinary tract
60% of colonized mothers birth colonized babies; Neonatal disease in 3/1000 live births
Risk factors:
- Immune status of mother is more important risk factor than exposure to organisms for acquiring neonatal disease (maternal type-specific capsular antibodies transplacentally passed to fetus is protective during first few months of life as infant's immune system matures)
- Heavy vaginal colonization during birth increases likelihood of neonatal colonization, but does not increase risk of disease
- Complement deficiency
- Pregnancy risks include: Premature birth; Prolonged rupture of membranes; Fever during delivery
Early onset neonatal disease: Within 7 days of birth
- Acquired in utero or during delivery
- Three times more frequent than late onset disease
- 15-30% of post-meningeal infants experience neurological sequelae that include blindness, deafness, and severe mental retardation
Late-onset neonatal disease: Occurring 1 week to 3 months after birth
- Acquired from exogenous source: Mother, other infants, health care provider
- Presents most commonly as bacteremia with meningitis; Neurological complications are common
Puerperal sepsis: Common cause of maternal death in pre-antibiotic era
Disease in nonpregnant adults
Risk Factors:
- Diabetes mellitus
- Cancer
- Alcoholism
Proportionally more adult disease, but incidence is higher in neonates
Foodborne disease: Infrequent foodborne disease outbreaks
Organisms multiply when contaminated foodstuffs are improperly refrigerated and allowed to stand at room temperature for several hours between preparation and consumption
Contamination of food is result of incomplete processing or unsanitary food handling by carriers (poor hygiene, ill or asymptomatic food handler) or unpasteurized milk (frequent outbreaks before advent of pasteurization)
High infectious dose of >107 organisms
Explosive common-source Group D outbreaks (2-36h incubation period) with a clinical syndrome similar to staphylococcal intoxication
Note: Septic sore throat, scarlet fever and other pyogenic and septicemic syndromes are also infrequently acquired from ingestion (low infectious dose of <1000 organisms) of contaminated food (onset after 1-3 days)
![]() Sequelae
of Acute Streptococcal Infection: Serious suppurative and nonsuppurative
sequelae in pre-antibiotic era; Nonsuppurative rheumatic fever and glomerulonephritis
is still important in developing countries
Sequelae
of Acute Streptococcal Infection: Serious suppurative and nonsuppurative
sequelae in pre-antibiotic era; Nonsuppurative rheumatic fever and glomerulonephritis
is still important in developing countries
Acute rheumatic fever (ARF)
Within 2-3 weeks (latent period) following respiratory infection only (e.g., pharyngitis)
For diagnosis, must demonstrate recent infection by culture or serology; Detect an increase in antibody titer to at least one of SLO, DNase B, hyaluronidase, streptokinase
Following epidemic pharyngitis: ARF in as many as 3%; Following sporadic pharyngitis: ARF in 1 per 1000
Acute post-streptococcal glomerulonephritis
Acute glomerulonephritis follows either respiratory (e.g., pharyngitis) or cutaneous streptococcal infection
Latent period: 1-2 weeks after skin infection and 2-3 weeks after pharyngitis
Associated with specific, well-defined group of serotypes
Incidence following infection varies from less than 1% to 10-15%
Most often seen in children
![]() Viridans
Streptococcal Infections: Streptococcus mutans is major dental pathogen
Viridans
Streptococcal Infections: Streptococcus mutans is major dental pathogen
Acidoduric (durable in acidic environment) and acidogenic (acid generating) properties, and the ability to synthesize extracellular adherent polysaccharides enable these organisms to establish initial colonization of dental surfaces and to provide a foundation layer for the formation of a complex biofilm known as dental plaque
Enamel caries is acid demineralization of enamel caused by lactic acid production by these bacteria during fermentation of sucrose or other carbohydrates and is dependent upon a variety of physical, chemical, and mechanical factors
Dental caries can be visualized as a disease state that occurs only when three factors or conditions co-exist. These three interdependent components are:
Status of host and teeth (sites that organisms can colonize, in particular solid surfaces and interfaces)
Specific microflora
Nutritional substrate (carbon and energy source)
Gingivitis and more severe periodontal diseases are a result of plaque-derived infection at the tooth and gum interface with loss of gum tissue and underlying bone
Pyogenic oral infections can be acute or chronic in nature, caused by mixed anaerobic infection of tissue by plaque flora, e.g., by trauma, invasive dental treatments, periodontal disease, or infected dental pulps
Lysogeny (Lysogenic Conversion)
Lysogenized bacteriophages may play key role in directing synthesis of various Group A streptococcal enzymes and toxins
Pyrogenic exotoxin (a.k.a., erythrogenic toxin): Phage-associated muralysins produced by both Group A and C streptococci
Grp C muralysin is N-acetylmuramyl-L-alanine amidase that lyses streptococcal cell walls; Used to produce L-forms (cells lacking rigid cell walls) or to purify membranes and M protein
Virulence Factors of Group A Streptococcus pyogenes: Structural molecules; Toxins; Enzymes
Cellular components
Lipoteichoic acid
Adherence to buccal epithelial cells
Cytotoxic for wide variety of cells
Colonization ligand: Forms complex network with M protein and binds via lipid moiety to fibronectin on epithelial cells
M protein
Antiphagocytic; alpha-helical coiled dimer; fibrillar molecule
Inhibits complement component C3b (Factor H, serum control protein) deposition on streptococcal cell surface, inhibiting alternate complement pathway and opsonization
Cell wall is potent activator of alternate complement pathway, but M-protein prevents these reactions
Grp A Strep with type-specific M-protein survive until type-specific antibody response develops
Amino-terminus (distal to cell) contains antigenically variable determinants; Three large tandem repeat regions contribute to antigenic diversity with intragenic recombination events
Abnormal host immune response against cross-reactive antigens may result in sequelae
F protein: Binds fibronectin of host; Major adhesin to throat and skin by mediating adherence to epithelial cells
Associated proteins: Some under control of virulence regulon and co-regulated with M-protein
C5a peptidase destroys chemotactic signals
Serum opacity factor
Fc receptor protein binds to Fc region of mammalian IgG
Antiphagocytic capsular polysaccharide
Hyaluronic acid mimics animal tissue ground substance found in host connective tissue and is therefore nonimmunogenic; assists in avoiding phagocytosis
Extracellular components
Hemolysins: Two hemolytic and cytolytic toxins
Streptolysin O (SLO)
Prototype of oxygen labile or thiol-activated bacterial cytolytic protein toxins produced by Streptococcus, Bacillus, Clostridium, and Listeria
Irreversibly inactivated by cholesterol
Bind to cholesterol-containing membranes and form arc- or ring- shaped oligomers that make cell leaky (RBC's, PMN's, Platelets,etc.)
SLO induces rapid antibody response
SLO titer indicates recent infection (300-500 in pediatric populations)
Streptolysin S (SLS)
Oxygen stable, non-antigenic
Extractable only in presence of carrier or inducer, e.g., serum, albumin, RNase-resistant fraction of RNA
Lytic for red and white blood cells and wall-less forms (protoplast, L- forms)
Responsible for surface hemolysis on blood agar plates; Inhibited by phospholipids
Pyrogenic exotoxins (a.k.a., erythrogenic toxins)
Produced by more than 90% of Grp A streptococci; 3 types Groups A, B, and C
Heat labile; Stable to acid, alkali, pepsin
Structural gene is carried by temperate bacteriophage, as is the case with diphtheria toxin
Result in fever and scarlet fever rash, increase susceptibility to toxic shock, cause reticuloendothelial system blockade, act as mitogens, myocardial and hepatic necrosis, decrease in antibody synthesis
Immunomodulators (superantigens) at low concentrations, stimulate T cells
Type C toxin increases permeability of blood-brain barrier to endotoxin and bacteria
Nucleases: Reduce viscosity
Four antigenic types (A,B,C,D) in S. pyogenes assist in liquefication of pus to generate growth substrates
Nucleases A, C have DNase activity
Nucleases B, D also have RNase activity
Require calcium and magnesium
Antibody titers to DNase B useful serodiagnosis
Other Enzymes
Two different streptokinases that catalyze conversion of plasminogen to plasmin, leading to digestion of fibrin (dissolve blood clots); may enable rapid dissemination through infected tissues
Hyaluronidase hydrolyzes hyaluronic acid; "spreading factor"
DPNase, cardiohepatic toxin, proteinase, NADase, ATPase, phosphatase, etc.
Virulence Factors of Group B Streptococcus agalactiae
Enzymes of unknown pathogenicity: Dnases, hyaluronidase, neuraminidase, proteases, hippurase, hemolysins
Immune Response Against Streptococcal Disease
Antibodies against type-specific capsular antigens are protective; Infants without type-specific maternal antibodies are at increased risk of acquiring infection
Bactericidal activity requires the presence of complement
![]() General
Overview
General
Overview
Gram stain of tissue sample can provide rapid initial diagnosis
Bacitracin sensitivity test for presumptively distinguishing between beta-hemolytic streptococci isolated from pharyngeal swabs (95% accuracy of Grp A strep sensitivity)
Negative catalase used to differentiate from Staphylococcus
![]() Group
A Streptococci
Group
A Streptococci
Specimen Collection and Processing
Throat swabs from the posterior oropharynx (back of throat, e.g., tonsils) or from skin lesion
![]() Microscopy:
Gram stain
Microscopy:
Gram stain
Cocci in short chains in clinical specimens; Longer chains seen in culture
![]() Culture
Culture
Primary culture by pour and streak plate
Fastidious growth requirements; Optimal growth on enriched blood agar; Growth inhibited by glucose in medium (fermented with lactic acid buildup)
1 to 2-mm domed white (grayish to opalescent) colonies with large zone of beta-hemolysis (several times that of diameter of colony) after 18-24h incubation
Colonies of encapsulated strains appear mucoid on moist media, wrinkled on dry media; Colonies of nonencapsulated strains appear small and glossy
![]() Identification
Identification
Preliminary identification
Positive CAMP test
Hydrolysis of hippurate
Antigen detection
Group Specificity
Positive identification of group-specific carbohydrate (rhamnose, N-acetylglucosamine, galactose)
Type Specificity
Type-specific capsular polysaccharide (sialic acid residue)
Type-specific proteins
Methods
Bacitracin sensitivity
Rapid identification tests: Based on extraction of Grp A carbohydrate directly from throat swabs
Coagglutination
Fluorescent Antibody
Antigen detection
Detection of group-specific carbohydrate (dimer of N-acetylglucosamine & rhamnose) (formerly C-Polysaccharide)
Capillary tube precipitin tests
Variety of agglutination tests
Detection of M protein by Capillary Tube Precipitin Test with extracts or whole cells
Detection of T protein by Slide Agglutination Test with trypsin treated whole cells; Adjunct to M-typing; routine surveillance
Antibody Detection
ASO Test: Detection of antibodies against streptolysin O confirm a recent Group A streptococcal infection
Detection of DNase B
Group B Streptococci
Microscopy: Gram stain
Cocci in short chains in clinical specimens; Longer chains in Cx
Culture: Large, buttery-appearing colonies usually surrounded by a narrow zone of hemolysis
![]() Therapy:
Aimed at prevention of suppurative complications and the nonsuppurative sequelae
of rheumatic fever and glomerulonephritis
Therapy:
Aimed at prevention of suppurative complications and the nonsuppurative sequelae
of rheumatic fever and glomerulonephritis
![]() Group
A Drug of Choice: Oral (PO) penicillin V (VK) or intramuscular (IM) benzathine
penicillin; Alternatives: Erythromycin, clindamycin, cephalexin (oral cephalosporin)
Group
A Drug of Choice: Oral (PO) penicillin V (VK) or intramuscular (IM) benzathine
penicillin; Alternatives: Erythromycin, clindamycin, cephalexin (oral cephalosporin)
![]() Group
B Drug of Choice: Intravenous (IV) penicillin G; Alternate: Vancomycin
Group
B Drug of Choice: Intravenous (IV) penicillin G; Alternate: Vancomycin
![]() High
MIC (minimal inhibitory concentration)
High
MIC (minimal inhibitory concentration)
![]() Antibiotic
tolerance has been observed
Antibiotic
tolerance has been observed
![]() Tolerance:
able to endure without effect
Tolerance:
able to endure without effect
![]() Acute
Rheumatic Fever
Acute
Rheumatic Fever
![]() Salicylates
and corticosteroids for acute symptom reduction and control of long-term sequelae;
Prevention by preventing initial strep infection or prompt treatment of pharyngitis
Salicylates
and corticosteroids for acute symptom reduction and control of long-term sequelae;
Prevention by preventing initial strep infection or prompt treatment of pharyngitis
![]() Acute
Post-Streptococcal Glomerulonephritis
Acute
Post-Streptococcal Glomerulonephritis
![]() Therapy
directed at secondary phenomenon of volume excess, hypertension, and seizures;
Sodium restriction, diuretics, anticonvulsants
Therapy
directed at secondary phenomenon of volume excess, hypertension, and seizures;
Sodium restriction, diuretics, anticonvulsants
![]() Must
demonstrate recent infection by culture or serology; Detect an increase in antibody
titer to SLO or DNase B
Must
demonstrate recent infection by culture or serology; Detect an increase in antibody
titer to SLO or DNase B
![]() Renal
biopsy, immunofluorescent exam, or electron microscopy to diagnose
Renal
biopsy, immunofluorescent exam, or electron microscopy to diagnose
(1).gif) Return to Pathogen List
Return to Pathogen List| Lecture Syllabus | General Course Information | Grade Determination |
| Laboratory Syllabus | Interesting WebSite Links | Lab Safety |